

After completing this unit you will:
* Although we use the commonly-used term ‘breaking bad news’ here, it might be better expressed as ‘delivering unexpected or potentially distressing news’.
If you work with women experiencing pregnancy loss you are likely to have to have difficult conversations with them when and/or after delivering bad or potentially distressing news.
Even if the initial news does not seem to cause upset, this may change over time. Information about next steps may be more upsetting than the diagnosis or it may compound it. Whatever the case, there are some conversations that are likely to be difficult or distressing for the woman.
Starting these conversations can be hard and upsetting. However, women tell us that they appreciate health professionals who are honest with them about what is going to happen and that clear information, sensitively given, can help them through.
I discussed with nurses what I could do with the baby and they were incredibly sympathetic and caring with their words, their tone and their time. They were also knowledgeable about what I could do with it, about bringing it back to the hospital.
We can all be better communicators. Good communication skills are key to obtaining information, conveying information, and enabling women to be able to take the decisions that are right for them.
Time spent listening helps you to understand the woman’s point of view and draws attention to her specific needs.
A simple, effective model of communication is the BEST model. It includes verbal and non-verbal ways of communicating along with emotional support.
* In the context of miscarriage, ectopic or molar pregnancy, we would use ‘end’ rather than ‘terminate’.
Communication starts even before we start talking. More than two thirds of a face-to-face conversation is based on body language. There is non-verbal communication from when you are first with someone in the clinic or consulting room. It is particularly important to pay attention to the non-verbal aspect of your communication when giving bad news to a woman. Eye contact is the strongest non-verbal gesture and indicates you are listening to the woman.
The doctor asked me if I had any more questions. I did, but she was looking at her watch, so I just kept quiet.
Information gathering is an art. You need to aim to actively guide the conversation, not by talking more or stopping the conversation, but by moving your discussion towards relevant topics at the same time as interpreting what the woman is saying to you.
If you are examining the woman, it may be helpful to talk to her while you do this, as long as you are talking about the examination or the problem. It may help put her at her ease.
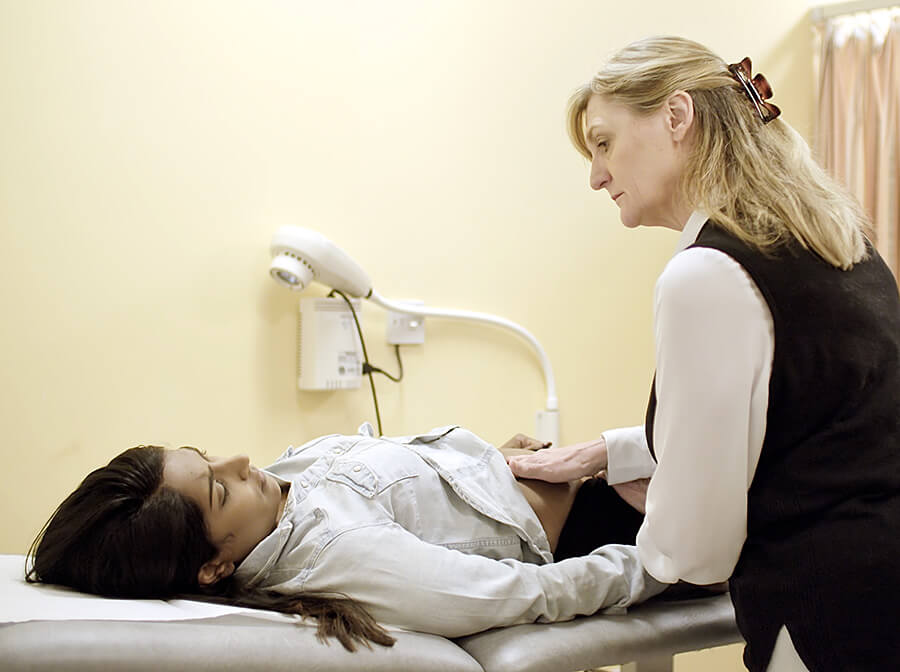
Women experiencing a pregnancy loss are likely to show a variety of emotions and may be distressed, withdrawn, disbelieving or even angry. How you communicate can make a significant difference.
Empathy is important in any trusting relationship. Your face, eyes, and gestures should all support you in demonstrating your continued interest in the woman. Listen to what she is saying and nod to show you are listening.
There is a Chinese proverb: ‘Words are just words and without heart they have no meaning’. Try to listen to the unsaid, be open to the expression of feelings and aim to enable non-verbal two-way communication.
It may be difficult, and possibly inappropriate, to try to end on a positive note when a woman is experiencing a miscarriage but it’s good to summarise briefly what you have discussed and ask if she has any questions.
You may find it useful to use phrases such as ‘I hope I have given you the information you need. Do you have any questions?’
* In the context of miscarriage, ectopic or molar pregnancy, we would use ‘end’ rather than ‘terminate’.
As you watch this, think about what these films tell you about the challenge of giving difficult news to women.
Consider whether this experience might be similar or different if a potential problem was identified during the anomaly scan.
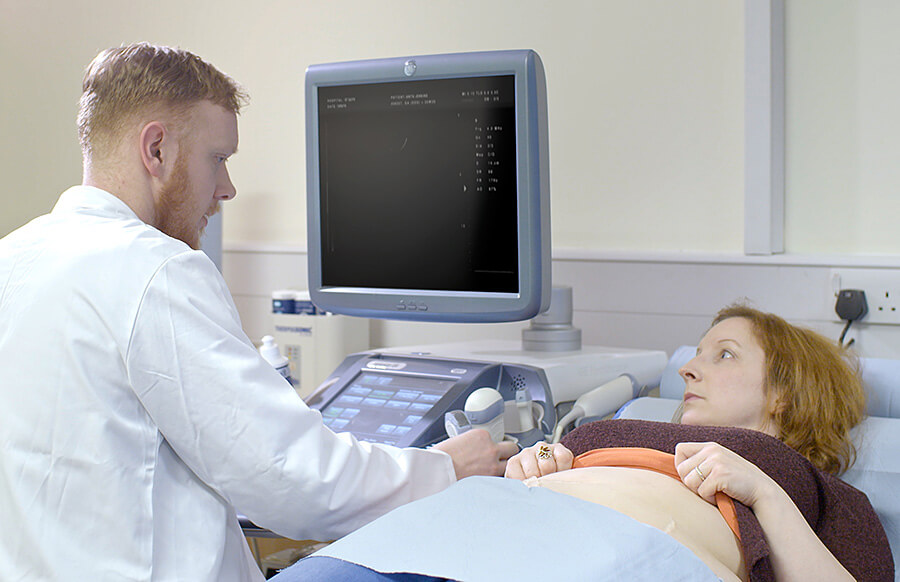
Routine dating or anomaly scans can be a time when a problem with a pregnancy is discovered. It can therefore be challenging for the health professional carrying out the scan, not knowing whether all will be well or not. Even if you do not perform pregnancy scans yourself, you may find it useful to think about the issues below.
This film follows a couple as they attend for their dating scan.
As you watch the film, think about how the sonographer could have made the experience more manageable for the couple. In the next screen we will explore ways the experience could be better.
You may have noticed that the sonographer did not adequately introduce herself, or the purpose of the scan. Setting the scene at the very beginning with every woman will help if you have to go on to break bad news.
Women may start to guess something is wrong if you go quiet and they are likely to find that silence very difficult to cope with. At the same time, you need time to assess scan images, especially if they suggest or confirm a problem. Good communication, clarity, honesty and sensitivity can help everyone involved.
Next we explore some of the ways in which you can help make the woman’s experience better.
I sensed there was something wrong because there was a very heavy silence that fell on the room.
There are a number of ways in which you can make the experience more positive, or at least more manageable, for the woman or couple. Click on the images below to find out more about what you can do.
We recommend that anyone delivering potentially difficult news reads the UK consensus guidelines for the delivery of unexpected news in obstetric ultrasound: The ASCKS Framework.
Talking with women about the disposal of pregnancy remains can be difficult and daunting, especially if you feel under pressure to gain consent for one of the options available. You must also ensure that know your hospital’s policy and practice* and have information with you, not just a check-list.
The woman may need time to consider options and you need to allow for this. Remember that she is likely to be distressed already, following confirmation of her loss and the need to make decisions about its management. She might be very shocked to be asked to consider what happens to the remains of her baby and find it impossible to think about this at this time – or at all. You should reassure her that she can make a decision at a later date if she prefers and let her know the timeframe for this.
If possible, provide at least written information about what option will be used if she does not make a decision and tell her whom she can contact if she changes her mind or would like more information.
Her wishes, or choice to opt out of decision-making, must be respected and clearly recorded.
* Note that legislation in Scotland on the disposal of pregnancy remains is different from that in England, Wales and Northern Ireland. See references at the end of this unit.
We wouldn’t expect a decision but we like to make them aware of their choices so they can have some time in thinking what’s right for them.
Think about how you could have helped Corinne and Erin to have a less traumatic experience.
Think about how you can integrate some of Rachel’s advice into your own practice and the importance of being familiar with national as well as local guidance and policy.